Skin Cancer Affecting Pigment - Making Cells
Melanoma affects melanocytes, the cells that make pigment that gives the skin its color. It’s not as common as other forms of skin cancer, but is much more likely to spread. In fact, its rate of spread to lymph nodes is up to 40%.
Melanoma is a leading cause of death from skin disease – more than 70% of skin cancer deaths are from melanoma – and, each year, it becomes more common. Men age 49 and under have a higher probability of developing melanoma than any other cancer. From ages 15 to 39, men are 55% more likely to die of melanoma than women in the same age group. Women age 49 and under are more likely to develop melanoma than any other cancer, except breast and thyroid cancers.
Prevention and Screening
On average, a person’s risk for melanoma doubles if they have had more than five sunburns, but just one blistering sunburn in childhood or adolescence more than doubles a person’s chances of developing melanoma later in life. The best way to prevent skin cancer is to always use sunscreen and to limit the time you spend in the sun.
- Use sunscreen with sun protection factor (SPF) of at least 30, even when you are going outdoors for a short time.
- Apply a large amount of sunscreen on all exposed areas, including ears and feet.
- Look for sunscreen that blocks both UVA and UVB light.
- Use a water-resistant sunscreen.
- Apply sunscreen at least 30 minutes before going out. Follow package instructions about how often to reapply. Be sure to reapply after swimming or sweating.
- Use sunscreen in winter and on cloudy days, too.
Use other measures to protect your skin from the sun:
- Ultraviolet light is most intense between 10 a.m. and 4 p.m. Try to avoid the sun during these hours.
- Wear wide-brim hats, long-sleeve shirts, long skirts or pants.
- Keep in mind that some surfaces reflect light, such as water, snow, sand, concrete and areas that are painted white.
- Remember that the higher the altitude, the faster your skin burns.
- Do not use sunlamps and tanning beds. Spending 15 to 20 minutes at a tanning bed does as much harm as a day spent in the sun.
Check your skin once a month. Have your doctor check it once a year if you are older than 40 and every three years if you are 20 to 40 years old.
Symptoms, Diagnosis & Outlook
Symptoms
Identifying melanoma at an early stage is important. Like all cancers, early detection can increase your chances for a cure. You may find it hard to tell if something on your skin looks like skin cancer. Organizations like the American Academy of Dermatology and the Skin Cancer Foundation have developed guidelines to help you examine your skin. Look for anything new, changing or unusual on your entire body, not just the parts that are exposed to the sun. In women, melanomas commonly appear on the legs, while men are more likely to see them on the trunk. However, melanomas can arise anywhere on the skin.
Most moles, brown spots and growths are harmless – but not always. Using the ABCDEs and the ugly duckling sign can help you detect melanoma.
The ABCDEs of Melanoma
Use the first five letters of the alphabet to help recognize the warning signs of melanoma:
- Asymmetry: most melanomas are uneven, or asymmetrical – one side is not like the other.
- Border: melanoma borders are usually uneven, with edges that may be scalloped or notched.
- Color: you shouldn’t see multiple colors in a common mole. Benign (noncancerous) moles are usually one shade of brown, but a melanoma may have different shades of brown, tan or black. You may also see red, white or blue as the melanoma grows.
- Diameter (or Dark): melanomas are usually the size of a pencil eraser (about 6 mm, or ¼ inch, in diameter) or larger when they are noticed, but can be smaller. You should also pay attention to a mole that is darker than others, but keep in mind there are also rare melanomas that are colorless because they have no melanin (amelanotic).
- Evolving: look for any change in size, shape, color, surface (lump or bump) or sensation. This includes any oozing, scales, bleeding, itching, or crusting, tenderness or pain.
If you notice these warning signs, or anything NEW, CHANGING or UNUSUAL on your skin, see a doctor who specializes in the treatment of skin, called a dermatologist, promptly.
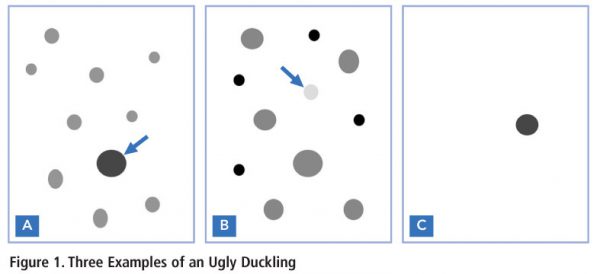
Do You See an Ugly Duckling?
What does an ugly duckling have to do with melanoma? An ugly duckling stands out from the others, and a mole that doesn't look like the others is an ugly duckling. Don't just look at individual spots, but also compare any moles that looks suspicious to other moles around them. “Ugly duckling” lesions might be lighter, darker, larger or smaller compared to surrounding moles. Or, they might be “lone ducks.” These are lesions that might look different in size or color, without any surrounding moles to compare them to.
Other warning signs are:
- A sore that doesn’t heal
- Spread of pigment from the border of a spot into surrounding skin
- Redness or a new swelling beyond the border of the mole
Be sure to show your doctor any areas that concern you and ask your doctor to look at areas that may be hard for you to see. It’s sometimes hard to tell the difference between melanoma and an ordinary mole, even for doctors, so it’s important to show your doctor any mole that you are unsure of.
Remember, too, that a small portion of melanomas start in places other than the skin, such as under a fingernail or toenail, inside the mouth or even in the colored part of the eye (iris), so it’s important for your doctor to check for any new or changing spots in these areas as well.
Sources: National Cancer Institute, Skin Cancer Foundation, American Cancer Society, American Academy of Dermatology
Diagnosis
Your Penn State Health dermatologist can diagnose and treat early-stage melanomas. However, high-risk or later-stage melanomas should be seen at Penn State Cancer Institute. How do you know where to go? Call your dermatologist and describe the spot you are concerned about.
To diagnose melanoma, the doctor will ask you to answer in-depth questions about your personal and family medical history and examine your skin using dermoscopy, which is a microscopic examination of the lesions.
If your doctor thinks you might have a melanoma or other skin cancer, he or she will remove all or some of the spot, called a biopsy. A pathologist will look at the skin sample under a microscope to check for cancer cells. If you have skin cancer, you may need more tests to see whether it has spread.
The treatment for melanoma depends upon its stage, which identifies how far advanced it is. Treatment can include:
- Surgery: the type of surgery depends upon the melanoma’s location and how deep it is. Early stage melanoma can be removed in the office while you are awake. Your doctor will remove some normal-looking skin around the tumor to make sure there are no other cancer cells. In many cases, this is the only treatment you will need.
- Radiation therapy: used to kill cancer cells or stop new ones from forming.
- Immunotherapy: a type of medication sometimes used after surgery to help your immune system seek out and destroy cancer cells that may remain. This may be the main treatment if surgery cannot remove the cancer.
- Targeted therapy: drugs designed to find cancer cells and attack them, which can temporarily shrink the cancer.
Melanoma and Skin Cancer Center
The Multidisciplinary Skin Cancer clinic at Penn State Cancer Institute specializes in treating melanoma and other skin cancers– even very rare ones.
Our specialists diagnose and stage melanoma and are experts in its treatment and recovery. Here, you’ll have access to all the latest therapies, as well as clinical trials testing new treatment methods. Team members meet regularly, along with radiologists, radiation oncologists and pathologists, to discuss cases as a group. These members and scientists also meet to discuss clinical trials and novel ideas for new studies.
Meet the Team
Why Choose Penn State Health for Care
Comprehensive, Compassionate Care
Penn State Health provides specialized testing, treatment and management for cancerous skin lesions. Our medical team is consistently recognized nationally through Best Doctors in America and America’s Top Doctors awards.
Leading-Edge Clinical Trials
The skin cancer experts at Penn State Health Milton S. Hershey Medical Center and Penn State Cancer Institute are committed to offering their patients the latest treatment options, including access to leading-edge clinical trials. Our superb clinical research team includes dedicated research nurses, clinical trial coordinators and data analysts and gives patients the opportunity to participate in the latest clinical trials. Learn more about new Penn State Health clinical trials at StudyFinder.
Support Groups
Support groups offer an opportunity to connect with other patients, caregivers and families. Learn more about support groups offered at Penn State Cancer Institute.
The Melanoma Support Group provides support to Stage 3 and 4 melanoma patients and their caregivers by sharing our experiences and practical information, while providing encouragement, hope, networking and educational opportunities. Structured meetings include introductions, sharing experiences and feelings, exchanging information and building a sense of belonging. Speakers and experts on topics of interest identified by the group members are also scheduled. We support melanoma research through advocacy and related activities.
For more information, please contact Carol Mallon, MS, RN, AOCNS at 717-531-5784 or Mary Ellen Loser, BSN, RN, CPSN at 717-531-1657.
Convenient Locations
Find the care your family needs, close to home, at one of our many locations throughout central Pennsylvania.
Find a location near you


